As competition becomes more and more intense, now more than ever, it is critically important to get your house in order with regard to instrumentation in your practice.
The entrance of franchisers into the marketplace and the continuing marketing aggression by existing operators has put the focus on every facet of the way in which optometrists conduct their business. Learning how to use every means available, not only to attract new clientele, but more importantly, retaining those already existing patients, is crucial!
First Impressions Count
Location, range of frames, retail appearance, advertising, staff and pricing, are just some of the aspects that determine whether a client decides to visit a practice. Deciding whether to entrust the practice with the care of their eyes is the next hurdle.
A consulting room’s eye examination equipment is often a neglected determinant in whether or not a practice creates a positive first impression. It’s not only the ragged upholstery on a consulting chair that will be initially noticed. For the seasoned patient, the lack of drops required when using a non-contact tonometer will certainly spark curiosity in some, while others will be impressed with the results of digital retinal photography.
The investment in new technology that allows examination techniques outside the realm of standard Medicare consultations, allows optometrists to have the opportunity to collect additional fees…the extra revenue generated will exceed any lease or hire purchase expenses
Creating the Scene
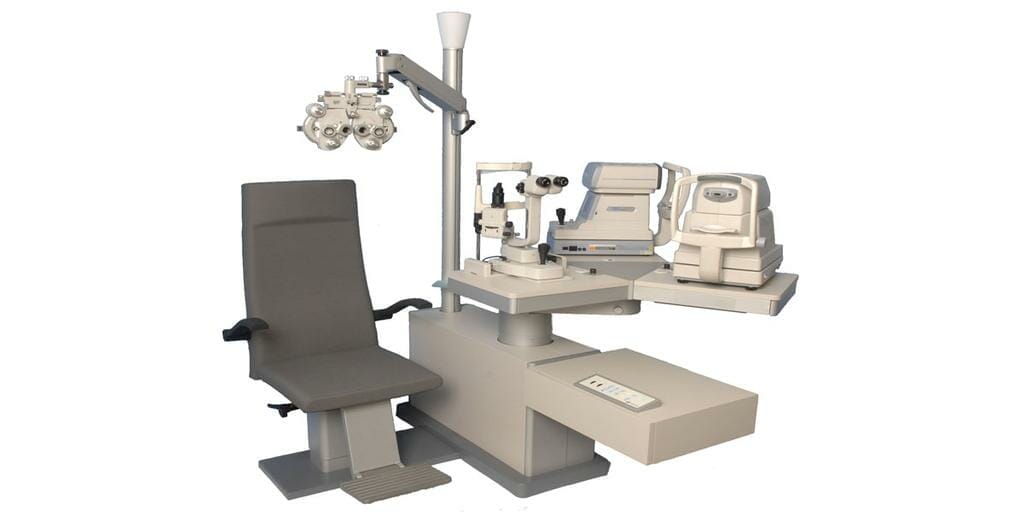
What constitutes a basic room these days and what extras are necessary to impress, attract and retain both new and existing patients?
Firstly, a chair and stand should allow the use of two or preferably three instruments in close proximity to the patient. Probably the most important item will be a slit lamp. Most practices have an auto-refractor/keratometer and more recently, are investing in the three-in-one or four-in-one instruments that incorporate the additional functions of tonometry (and pachymetry).
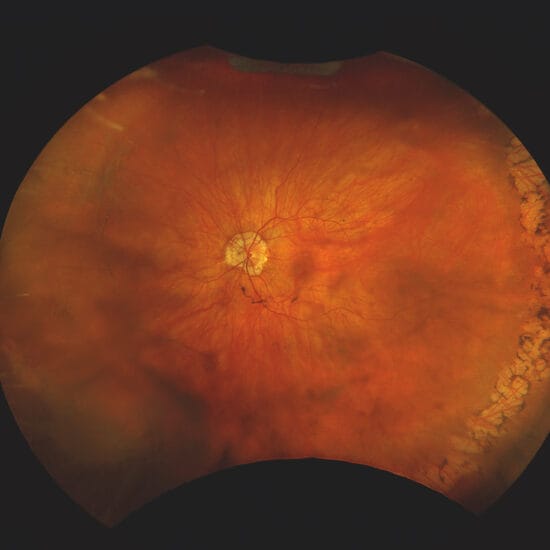
If the third position allows for an additional instrument, most practices are now including a retinal camera for use on most patients. Retinal cameras have now become a standard item in Australian clinical practices rather than a luxury.
A refractor head, or vision tester, has also been a normal fixture in consulting rooms for decades, replacing the trial frame and lenses as the main mode of refraction by the optometrist. However, the mechanical type of refractor is now increasingly being replaced by computerised, automatic refracting units which can be operated by means of a manual console on the practitioner’s desk. These systems create greater comfort for the optometrist, particularly in the shoulders. They can also integrate with lens meters, auto refractors, and LCD chart, with results then sent to the consulting room PC to be installed into the practice management system. This not only adds to the efficiency of the consultation, but eliminates data entry errors that tend to occur with less automated systems.
Integrating IT
Following the changes with Medicare to include a separate item number for perimetry, most practices have a visual field screener. Given the need for computerised integration of bowl perimeters, modern perimeter designs produced by such suppliers as Optoglobal and Medmont are considerably easier to integrate into your practice IT system than ever before, requiring far less maintenance than former models. Specialised capabilities such as flicker perimetry and SWAP (blue on yellow) perimetry, enables the optometrist to gain a greater sensitive assessment and superior assistance with diagnosis, than ever before.
Hand-held equipment has come a long way since many of us first bought our instruments in the last century! Advances in battery and bulb technology have significantly improved modern ophthalmoscopes and retinoscopes. Furthermore, contemporary BIOs are a far cry from the basic restrictive models that were available as recently as the start of this decade. The best BIOs are currently unplugged; therefore, the battery is mounted at the back of the crown to prevent unnecessary cables hanging from the BIO, eliminating the need to carry around external power supplies. They are lightweight, have more filters than the average optometrist will ever need and have optics that lift away if you want to have a conversation with your patient without readjusting your alignment.
The humble lensmeter, fundamental to every practice, has also undergone a technological revolution. While the old fashioned, down the barrel vertometer / focimeter still works perfectly well, many practices are now opting for computerised lensmeters. These measure all types of lenses, including progressives. They provide a print-out of the spectacle power if necessary, and as described above, can interface with automatic refractors and practice management systems.
Deploying the Big Guns
A new generation of instruments is giving the practitioner an unprecedented ability to analyse specific structures of the eye. Optometrists who want to gather additional information about the anterior eye have recently rejected their keratometer in favour of a corneal topographer. However, there is now a choice of instruments, such as Topcon’s CA-100 Corneal Analyser and the Oculus Pentacam, which give exceptional data about aspects of the anterior eye, including: topography and elevation maps, corneal wavefront analysis, pachymetry, analysis of the anterior chamber and measurement of the pupil under photopic, mesopic and scotopic conditions.
Capturing images of the anterior eye can now be achieved using digital cameras that integrate with the slit lamp. The Topcon DC-3 is streamlined and unobtrusive to the practitioner and allows the capture of still or video imaging to be sent directly to the PC for analysis and storage.
For the technologically savvy optometrist, a plethora of instruments are available for focusing and treating the posterior eye. In recent years, the GDX from Carl Zeiss, has allowed assessment of the nerve fibre layer. However, the emergence of ocular coherence tomography (OCT) more recently, has revolutionised the practitioner’s ability to analyse the posterior eye in extreme detail.
Using the Topcon’s spectral domain 3D-OCT, without mydriasis, the optometrist can now examine a slice of retina in three dimensions and overlay this with images captured by the internal retinal camera. This produces an unprecedented view of not only the nerve fibre layer, but also the macula and other retinal structures. This goes beyond what is presently achievable using direct or binocular indirect ophthalmoscopy.
Essential Upgrades
Most optometrists report that the investment in new or upgraded equipment is not only impressive to patients, signifying the practice is up to date, but also improves the enjoyment of their position and boosts the quality of the practice. Also, the investment in new technology that allows examination techniques outside the realm of standard Medicare consultations, allows optometrists to have the opportunity to collect additional fees. In virtually all practices that invest in new technology, the extra revenue generated will also exceed any lease or hire purchase expenses.
The decision to upgrade equipment should not be a question of if, but rather, when.
Lee Pepper is the consultant optometrist with Optical Manufacturers in Sydney. His role is to give advice to practitioners with varying knowledge of technology about consulting room equipment options. He can be contacted at lee@omf.com.au.