Following his eventful vitrectomy, Professor Nathan Efron is troubled by a small but annoying blind spot on his personal journey of retinopexy, cryopexy, vitrectomy and IOL surgery.
Now that’s one hell of a melodramatic title for a blog, and it comes with a warning: if you are the type that gets nightmares after reading scary stories, you might just want to skip over this article and read on.
Avid followers of miblog will recall that the last instalment ended with my observation that, following my right eye vitrectomy revision procedure, I noticed a kind of ‘after-image’ just below the point of fixation. I was first aware of this visual anomaly during the immediate post-operative recovery phase, when my vision was about 6/18. Both Mike and Bill quite confidently proclaimed that vision is often disturbed following a vitrectomy and epiretinal membrane peel, and that vision can take anything from six to 18 months to return to normal.
Aside from the after-image, which I shall explain in more detail a little later, my vision just didn’t seem quite right. Mike mentioned to me that patients who have had the same procedure often reported imperfect vision, and some have stated that the quality of vision is akin to watching a high definition television screen with lots of pixels missing. Well, that’s exactly how it seemed to me.
And here’s the spooky bit… this blind spot was in the form of a flying or winged angel…
Finding an Explanation
I figured if many patients complain of sub-optimal vision following an epiretinal membrane peel, then there must be something in the literature about this. Certainly patient blogs referred to imperfect vision following this procedure, but I wanted some hard evidence, and good explanations. Sure enough, I found one paper where the authors concluded “Although visual acuity and macular edema were improved after… (a vitrectomy and epiretinal peel)…, macular function, as indicated by multifocal electroretinography, had limited recovery at 12 months”.1 They added “This incomplete recovery may explain patients’ reports of blurred vision despite relatively good visual acuity after epiretinal membrane peel surgery”.
So, this had me quite worried. Was I really going to have some form of visual defect for the next 12 months? Or even worse, was I going to be stuck with this anomaly forever? Lim and colleagues were unable to identify the precise cause of the abnormal retinal responses they observed.1 Whatever the answer to these unknowns, I decided to set out to try and determine the extent of my apparent visual compromise, and contemplate the cause.
First, I thought I would take a look at my pre- and post surgery optical coherence tomography scans (Figure 1). Compared to the pre-surgical scan, my retina appeared a little ‘spongy’ and oedematous after surgery. However, the macula was still well-defined and attached, and certainly Mike and Bill did not seem at all concerned.
A Curious Apparition
Back to the ‘after image’. A month or so after the vitrectomy, my vision had returned to 6/5+, but the world was still ‘pixel deficient’ and I was still aware of this persistent after-image, especially when I went looking for it. I soon discovered that this was a small blind spot, just infero-temporal to my point of fixation. I could clearly and accurately make out the shape of this blind spot by looking at a fixation point on an otherwise blank field and blinking rapidly.
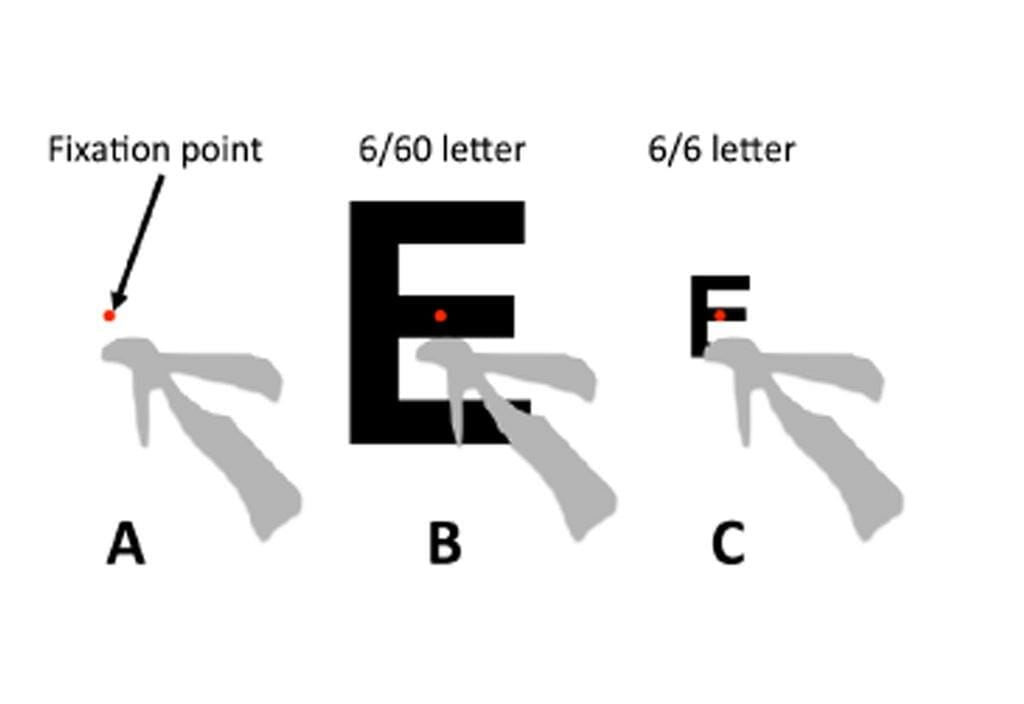
And here’s the spooky bit… this blind spot was in the form of a flying or winged angel (Figure 2). Given that it was also black and presumably represented a defined region of ‘dead’ receptor cells, I immediately coined the term ‘flying angel of death’ to describe it.
You might be wondering how I could see 6/5+ given that my flying angel of death partly obscures a 6/6-sized letter, as shown in Figure 2c. The answer must be ‘microsaccades’. Thus, when I stare at a 6/6-sized letter, natural tiny eye movements allow a rapid scanning of all parts of the letter, allowing me to establish that it is an ‘E’, rather than, say, an ‘F’. Thus, I consider my right eye visual acuity to be a ‘slow 6/5+’.
I experienced similar problems reading. Because my flying angel of death sits to the right of my fixation point, upcoming text is partially obscured as I scan from left to right while reading. So, although I can read small print, I consider myself to be capable of reading a ‘slow N6’.
I took my artwork depicting my flying angel of death to show Mike and Bill. They were somewhat perplexed. Bill asked “Is it really that big?” I explained it was; that it seemed to be about the size of a 6/60 letter on an eye chart viewed at 6m, but that it fortunately did not overlap the macula. Both Mike and Bill again expressed their confidence that this would go away before long. Every time I presented for an examination after that, they asked me if I was still troubled by my flying angel of death.
More Blind Spots
After a while, I sensed that my visual deficit was a little worse than first thought. I couldn’t really see any gaps in the Amsler Grid, so I developed my own more sensitive technique of exploring my visual field. I simply fixated on a red spot while moving a ball point pen slowly around my central field, concentrating on observing the tip of the pen. Sure enough, I detected another small area of reduced visual sensitivity, along the mid-line on the nasal side.
To check out this field loss more thoroughly, I asked Suzanne to perform a field test on me, so she did a Medmont fast-threshold full-test. The results, shown in Figure 3, not only confirmed the location of my flying angel of death and the nasal defect, but also found a small superior-temporal defect (which I couldn’t really locate with my pen test).
The small nasal and superior field defects were not really noticeable when looking around generally, but probably explain the notion of ‘missing pixels’. However, the flying angel of death was really worrying, especially since I was still seeing it three months after surgery.
As to the cause of these visual defects? My guess is that when an epiretinal membrane is peeled away, minor damage can occur to the underlying retina. Based on extensive comment on internet patient forums of poor vision following this procedure, as well as my own experience, I suspect that epiretinal membrane peels carry a substantial intrinsic risk of minor visual decrement, which has yet to be fully documented in the literature.
Anyway, all I could do now was play a waiting game to see if Bill and Mike would be right in predicting that this would go away in 12 to 18 months.
Professor Nathan Efron is a researcher at the Institute of Health and Biomedical Innovation and School of Optometry and Vision Science, Queensland University of Technology. He is currently president of the Australian College of Optometry and vice-president of the International Society for Contact Lens Research.
Reference
1. Lim JW, Cho JH, Kim HK. Assessment of macular function by multifocal electroretinography following epiretinal membrane surgery with internal limiting membrane peeling. Clin Ophthalmol 2014; 4: 689–694.