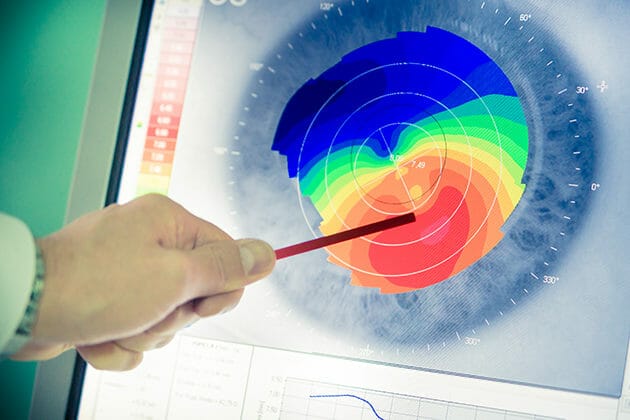
Keratoconus management has come a long way and we can now offer patients real hope with regard to preserving and even correcting vision. Careful patient selection is essential and multidisciplinary care is accepted as the gold standard to achieve optimal patient outcomes.
Keratoconus (KCN) is a chronic, debilitating, progressive corneal disease characterised by corneal thinning, protrusion and scarring, irregular astigmatism and poor vision. Although bilateral, the disease is asymmetrical and one eye will be affected more than the other. The incidence of KCN is about one in 2,000, increasing to one in 500 in the Asian population.
Progression often halts, or at least slows, in patients in their 30s or early 40s. However, it’s not unheard of for some to show continued progression into their 50s. Clinicians tend not to consider surgical treatment for patients over 30 (even less so for those over 35), unless there is definite evidence of progression. However, a paper presented at the RANZCO 2017 Congress reported that 18.5 per cent to 37 per cent of KCN patients aged over 30 did in fact progress significantly in at least one eye (>1.0 D in one or more parameters).1
These patients did not wear contact lenses (i.e. had relatively mild disease) and were presumed to be non-progressive. In light of this evidence, there is a strong argument for longer-term follow-up in the primary setting.
TREATMENT OPTIONS
Glasses are generally sufficient to manage KCN in the early stage. However, progression inevitably necessitates other treatment. Options include soft or rigid gas permeable contact lenses (CLs), or surgery such as intracorneal ring segments (ICRS – e.g. Kerarings), collagen cross-linking (CXL), topographyguided photorefractive keratectomy, toric phakic IOLs and penetrating keratoplasty (PK).2
While visual outcomes following corneal transplant are often good, there are significant risks and adverse events to consider (e.g. cataract development, glaucoma, graft failure and microbial keratitis). PK is therefore reserved as a last resort and used in approximately 20 per cent of KCN patients.3
I personally like to use Kerarings to restore corneal shape and visual function and/or CXL to stop progression where possible. Most patients are highly satisfied with the end results in my experience. Kerarings are better tolerated than CLs and can actually help improve CL tolerance.4 The rings do not permanently alter the corneal tissue, and are removable and exchangeable. Recovery is quick, with minimal down time. For patients with less than 3 D of astigmatism, I use CXL by itself. Where the level of astigmatism is higher, I usually combine it with Kerarings placement. All surgery carries a risk of infection or complication, which is why careful patient selection and benefit/risk assessment is essential.
Importantly, even though CLs do not involve surgery, they are not without risk. Correct use and care of the lenses is one of the biggest concerns, with ocular nfection and trauma a common occurrence. Gas permeable lenses have been linked to a reduction of corneal basal epithelial cell and anterior stromal keratocyte densities, while piggybacking CLs may be associated with corneal neovascularisation and giant papillary conjunctivitis.2
It’s likely that patients with KCN will be managed at some point by an optometrist. This, coupled with a lack of accepted referral guidelines, means that we (ophthalmologists and optometrists) must take care to prevent the possibility of suboptimal patient care.
PATIENT SELECTION
Let’s review the key factors to consider when deciding whether or not to refer a patient with KCN.
Early identification of patients is crucial to optimise surgical outcomes and protect/improve vision
Help Patients Make Informed Decisions
As healthcare professionals, we have a duty of care to help patients make informed decisions about their treatment. Optometrists are often taught to exhaust all CL options and/or wait for signs of disease progression before referring. This made sense when PK was the only surgical option, however, with the advent of newer therapies, it is questionable whether this referral paradigm still meets the best interests of patients.
ICRS and CXL can stabilise KCN progression to delay or even remove the need for PK. Studies have shown that vision improves by an average of also improve with CXL, although the latter is not primarily intended for vision correction. Dr. Alex Poon, Dr. Rosalind Stewart and I recently confirmed this with data from 36 patients (41 eyes), where uncorrected visual acuity (VA) improved by 2.55 +/- 2.88 Snellen lines (p < 0.005) following Kerarings with or without CXL. Clinical significance was reached for all endpoints in this series of patients (p < 0.005).5 Presented by Dr. Stewart at the RANZCO 2017 Congress, the findings were well received and are to be published. In short, we can generally reduce the patient’s dependence on glasses or contact lenses, with some achieving complete freedom. Neither procedure precludes future use of CLs or IOLs.
Early identification of patients is crucial to optimise surgical outcomes and protect/ improve vision. ICRS and CXL in patients with milder disease is associated with more consistent results and better visual outcomes, while the risk of corneal thinning, scarring, hydrops and corneal transplant can increase if surgery is delayed. Waiting for signs of progression before offering referral could potentially limit treatment options for the patient. Prompt referral to a specialist corneal surgeon for initial evaluation is therefore critical.
Even if they are suitable for surgery, some patients that I see prefer to continue with CLs or glasses. The point is that they are aware of all the options available to them and can make an informed choice.
Refer younger patients immediately
KCN in patients less than 18 years old tends to be more severe and progress faster. Immediate referral to a corneal specialist is always indicated in these situations.
Consider Patient Quality of Life
The Collaborative Longitudinal Evaluation of Keratoconus (CLEK) study found, unsurprisingly, that KCN negatively affects quality of life (QoL) and declines over time. Interestingly, the adverse effect is not proportional to clinical parameters such as visual acuity (VA).6 The study also showed significantly impaired vision-related QoL on par with patients who have advanced age-related macular degeneration, indicating how debilitating KCN can be.6
QoL has been shown to significantly improve in patients whose dependence on glasses or CLs is reduced or eliminated (i.e. following refractive surgery), particularly if they were heavily reliant on these vision aids previously.7,8 Likewise, studies have also confirmed that CXL and ICRS procedures have a positive effect on QoL.9-11
The increasing trend towards patient-centred care, rather than a one-size-fits-all approach, dictates that healthcare professionals treat the person as a whole and empower patients in the decision-making process. Using visual metrics alone to guide treatment is no longer adequate and QoL is rightly gaining increasing importance in treatment paradigms.
Below are some of the QoL considerations specifically relevant to KCN patients.
Patient Lifestyle
Given that KCN is a younger person’s disease, understanding the patient’s lifestyle – whether current or desired – is important. At this age, patients are often involved in physical and/or outdoor activities (e.g. water sports, camping, hiking), social activities and work/study. The burden of CLs and/or glasses can reduce, restrict or even rule out participation in one or more of these pursuits. Patients may feel self-conscious or even have anxiety issues. CL wearers frequently revisit for prescription changes and fittings, which can become burdensome. Some patients report dissatisfaction with the number and/ or bulkiness of items they need to keep on-hand in their lens kit.
Contact Lens Intolerance (CLI)
The definition of Contact Lens Intolerance (CLI) is broad and subjective – it might be physical or psychological; it might be continuous, intermittent or sporadic; it might be the result of inappropriate lens care or the presence of a co-existing condition. Common signs of intolerance include irritation, discomfort, dry eyes and seeing halos or ghost images. Tolerance can also be affected by circumstances out of one’s control (e.g. allergies, windy conditions, eye infection). CLI can even develop despite previous long-term tolerance by the patient.
I would argue that CLI also includes an inability to wear one or both lenses for the entire waking time. Contact lenses may be considered ‘well tolerated’ if the patient can wear them for eight to 10 hours a day to coincide with normal work/school/day activities. However, total waking time for many people is around 16 hours a day (assuming eight hours of sleep). This begs the question of how patients are supposed to cope with significant visual impairment for a substantial portion of the day if they cannot revert to wearing glasses. I think Gabriel Acevedo depicts it nicely in his cartoon (Figure 1).
Post-operative CL Fitting
ICRS placement is intended to improve the corneal surface regularity through its arc-shortening effect. Research indicates that fitting contact lenses is therefore easier following surgery, and this has been the experience of a number of CL specialists that I speak to. However, some optometrists have found the opposite to be true. The release of larger-diameter lenses has certainly helped to counteract this problem, which would be hard to justify as a valid reason for delaying referral for a surgical opinion.
Optimise the Better Eye
Research shows that maintaining vision in the good eye is critical to maintaining overall QoL.12 Low vision in the better eye results in poorer scores for social functioning and mental health, and role difficulties when compared to healthy controls.12
In the CLEK patient population, KCN diagnosis was common in early life but aggressive treatment was postponed until later in life when disease severity had worsened. Yet, the current evidence base supports early detection and management to prevent significant visual loss (as well as a concomitant reduction in QoL). With today’s treatment options, we are much better placed to stop disease progression and protect patients’ vision.
Define Disease Progression In The Context of Referral
A 2015 study found that local KCN referral patterns in NSW optometry practices varied and included the following:13
• Immediate referral for possible treatment
• No set time for referral
• Referral if progression of corneal biomicroscopic and topographic signs
• Referral based on a combination of factors
• Referral based on VA.
Nearly two-thirds of respondents referred for a surgical opinion when VA was between 6/9 and 6/12. However, 21 per cent waited until VA reached 6/18 before referring.13
Reaching consensus about the triggers for referral is clearly important (if not offered straight away).
Embrace Patient Co-management
Multidisciplinary care is accepted as the gold standard to achieve optimal patient outcomes. Some optometrists and ophthalmologists already co-manage various patients with eye issues – and KCN should be no different. I often work with a number of optometrists to jointly manage patients with KCN. Some post-operative patients continue to require CLs and the optometrist’s expertise in prescribing and fitting these is an important determinant of the overall outcome.
Where patients choose to continue with CLs and delay surgery, the referring optometrist often continues to liaise with me to ensure a timely review is conducted when progression becomes evident. The trigger for review in these cases is determined on a case-by-case basis, depending on the patient’s wishes and severity of disease. Access to a high-quality topography unit is strongly recommended when monitoring the corneal surface.
HOPE FOR THE FUTURE
KCN management has come a long way and we can now offer patients real hope with regard to preserving and even correcting vision. Optimising surgical outcomes relies on careful patient selection. If patients are not referred early enough, their options may be limited. With the availability of effective and safe procedures, such as ICRS and CXL, tailoring treatment to the individual patient has never been more important.

This is the way Keratocat reads and uses his phone after removing his contact lenses. Source: Keratoconus Group
Dr. Tess Huynh MBBS FRANZCO is a highly respected cataract, corneal and refractive surgeon with over 16 years of experience. Her significant cataract expertise allows her to perform both routine operations as well as more complex cataract surgery for patients with co-occurring eye conditions. Dr. Huynh also specialises in corneal conditions – she has a particular interest in collagen cross-linking to treat keratoconus, pterygium surgery using auto-grafting and corneal transplantation, including all types of lamellar surgery. Additionally, Dr. Huynh performs laser eye surgery (LASIK, SMILE and ASLA/PRK) and treats more general eye conditions. She is actively involved in research, teaching and charity work.
References:
1. Gokul, A., Patel, D. V., Watters, G. A. & McGhee, C. N. J. The natural history of corneal topographic progression of keratoconus after age 30 years in non-contact lens wearers. Br J Ophthalmol 101, 839-844, doi:10.1136/ bjophthalmol-2016-308682 (2017).
2. Moschos, M. M. et al. Contact Lenses for Keratoconus-Current Practice. Open Ophthalmol J 11, 241-251, doi:10.2174/1874364101711010241 (2017).
3. Barnett, M. Keratoconus: When to Fit Contact Lenses Versus Refer for Surgery. Contact Lens Spectrum (Accessed online 20 October 2017).
4. Ambrosio Jr, R. Kerarings in the clinic. The Ophthalmologist (Accessed online 20 October 2017).
5. Stewart, R., Huynh, T. & Pool, A. Keraring intrastromal corneal ring implants with/without crosslinking in the management of keratoconus [abstract]. 49th Annual Scientific Congress of the Royal Australian and New Zealand College of Ophthalmologists S37 (2017).
6. de Freitas Santos Paranhos, J., Avila, M. P., Paranhos, A., Jr. & Schor, P. Evaluation of the impact of intracorneal ring segments implantation on the quality of life of patients with keratoconus using the NEI-RQL (National Eye Institute Refractive Error Quality of life) instrument. Br J Ophthalmol 94, 101-105, doi:10.1136/bjo.2009.161562 (2010).
7. Shams, N., Mobaraki, H., Kamali, M. & Jafarzadehpour, E. Comparison of quality of life between myopic patients with spectacles and contact lenses, and patients who have undergone refractive surgery. J Curr Ophthalmol 27, 32-36,doi:10.1016/j.joco.2015.10.004 (2015).
8. Leong, A., Rubin, G. S. & Allan, B. D. Quality of life in high myopia: implantable Collamer lens implantation versus contact lens wear. Ophthalmology 116, 275-280, doi:10.1016/j.ophtha.2008.09.020 (2009).
9. Cingu, A. K. et al. Impact of Collagen Cross-linking on Psychological Distress and Vision and Health-Related Quality of Life in Patients With Keratoconus. Eye Contact Lens 41, 349-353, doi: 10.1097/ICL.0000000000000129 (2015).
10. de Freitas Santos Paranhos, J., Avila, M. P., Paranhos, A., Jr. & Schor, P. Visual perception changes and optical stability after intracorneal ring segment implantation: comparison between 3 months and 1 year after surgery. Clin Ophthalmol 5, 1057-1062, doi:10.2147/OPTH.S23147 (2011).
11. Wu, Y. et al. Rigid gas-permeable contact lens related life quality in keratoconic patients with different grades of severity. Clin Exp Optom 98, 150-154, doi:10.1111/
cxo.12237 (2015).
12. Sahebjada, S. et al. Impact of keratoconus in the better eye and the worse eye on vision-related quality of life. Invest Ophthalmol Vis Sci 55, 412-416, doi:10.1167/
iovs.13-12929 (2014).
13. Hodge, C. et al. Therapeutic treatment of keratoconus: a survey of local optometric practice criteria. Clin Exp Optom 98, 312-318, doi:10.1111/cxo.12233 (2015).










