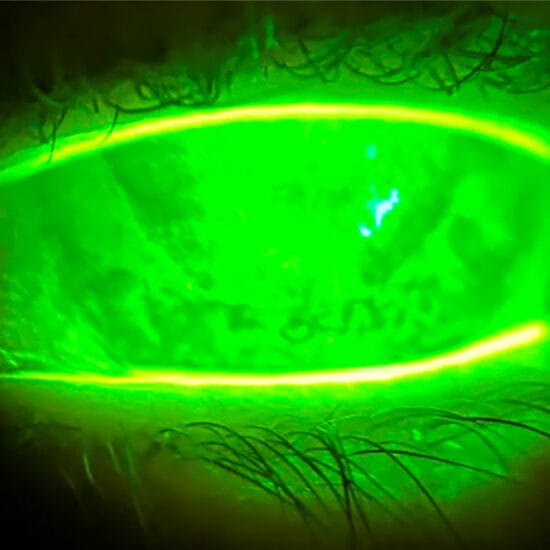
Convincing patients to listen to our advice, and the necessary precautions to protect their eyes and eyelids from harmful UV radiation, is a constant challenge.
As eye care professionals, we are very aware of the risk of ocular sun damage for our patients. Ultraviolet radiation damage can have serious vision-threatening and even potentially life-threatening consequences.
To tailor a recommendation… consider factors such as individual genetic makeup, family history of UV related conditions, and physical characteristics
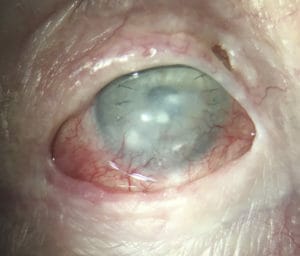
Figure 1. Dorothy, with a bandage contact lens in place, following reconstruction of a pseudo-lid using skin from her arm. Corneal graft failure left her with severe corneal
neovascularisation and corneal loss of transparency.
But how do we make patients ‘see the light’ and follow our professional advice about UV protection?
I believe the best way is to take a personalised approach:
- Show patients any signs or concerns youhave detected during their eye exam, and
- Give specific recommendations aroundUV protection, tailored to their individualcircumstances.
To tailor a recommendation on appropriate UV protection, consider factors such as individual genetic makeup, family history of UV related conditions, and physical characteristics. This is especially important if your patient is fair skinned or if their level of pigmentation, or any pre-existing UV damage, pigmentary lesions, or UV related ocular conditions, puts them at higher than average risk. Additionally, it is particularly important if they spend a lot of time outdoors while at work or leisure.
OCULAR UV DAMAGE
In the short term, overexposure to UV can lead to UV keratitis, and in the long term, patients can be susceptible to anterior ocular tissues such as pingueculae, pterygia, ocular surface squamous neoplasia and conjunctival melanoma. As we go deeper, UV radiation is associated with the acceleration of cataracts, and even deeper in the ocular tissues, UV radiation is associated with the development of choroidal melanoma and may possibly increase the risk of retinal damage from age-related macular degeneration.1
Unknown to many is that approximately 10% of all skin cancers occur in the delicate skin on the eyelids.2,3 Specifically, basal cell carcinomas are the most frequently encountered type of eyelid tumour, representing approximately 90–95% of eyelid tumours, followed by squamous cell carcinoma, sebaceous cell carcinoma, and malignant melanoma.4
While basal cell carcinomas are known to grow slowly and do not often metastasise, if undiagnosed and left untreated, they can be very destructive, extending into deeper layers of the skin and invading periorbital tissues and bone.4
Consequently, the skin surrounding the lids, particularly the lower lids and the skin surrounding the orbit, needs to be carefully shielded from the sun’s harmful rays in order to decrease the chance of cancerous growths in these areas.
Eyelid tumours need to be removed early to minimise damage to nearby ocular structures. However, early detection can often be challenging as eyelid tumours tend to grow inwardly under the skin,2,3,5 and may continue to grow in this inward pattern for many years before they are visible on the surface.2,3,5
CASE STUDY – DOROTHY*
Dorothy is a lovely 87-year-old who has been seeing me for the past few years. Her daughter says Dorothy was always out in the full sun hanging out the family washing, and, as consistent with the era, did not wear hats or sunglasses or use sunscreen to protect her skin.
Unfortunately, Dorothy had developed an extensive basal cell carcinoma involving her right cornea, the skin of her right eyelids, and to some extent, the skin on her upper right cheek.
In order to reconstruct Dorothy’s eyelid following removal of cancerous tissue, her oculoplastic surgeon used skin from her arm. Given the extensive nature of the basal cell carcinoma on her cornea, she also underwent a corneal transplant.
Dorothy was referred to me to support her corneal surgeon and oculoplastic surgeon by providing her with a bandage contact lens to maximise the comfort of her very sensitive ocular surface, epilate ingrown eyelashes, and optimise the limited remaining vision of her left eye, which had advanced macular degeneration.
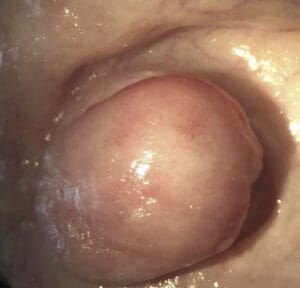
Figure 2. Dorothy’s eye was eventually surgically
occluded with skin to give her relief and comfort
from her ocular pain.
Unfortunately, despite several corneal transplants, none of the procedures were successful. Dorothy’s right eye, even with a bandage contact lens, was always watery and in constant pain. Eventually, her eye was surgically occluded to minimise her ocular pain.
Despite receiving the best professional care, under multiple surgeons, Dorothy’s quality of life has been profoundly negatively impacted due to the extensive damage caused by basal cell carcinoma.
Dorothy’s case emphasises that we have a strong duty of care to help prevent UV damage by educating all of our patients about the importance of UV protection. We must also do our best to prevent the progression of any existing UV associated ocular conditions we detect in our patients.
HERE COMES THE SUN… ADVICE TO PATIENTS ABOUT UV DAMAGE
As optometrists we can empower our patients to live a healthy lifestyle while avoiding unnecessary UV damage and protecting themselves against harmful UV rays.
Our recommendations can include general diet advice, including dietary supplements where appropriate for macular degeneration, as well as tailored advice that takes into consideration our beach culture and predominantly outdoor lifestyle, as well as the patient’s age, skin type, family and medical history, work and leisure interests.
It is important, at every opportunity, to remind patients to take precautions when outdoors by using sunscreen, wearing a hat and UVA and UVB protective wraparound sunglasses (and snow goggles when appropriate). Any diagnosed conditions require appropriate early management and reassessment.
In summary, by providing each patient with a personalised recommendation, as well as the reasoning behind our recommendation, patients are more likely to pay attention to our advice and protect themselves from UV radiation.
*Patient name changed for anonymity.
Margaret Lam is currently the National President of the Cornea and Contact Lens Society of Australia, a National Director of Optometry Australia and a Director of Optometry NSW/ACT and teaches at the School of Optometry at UNSW as an Adjunct Senior Lecturer. She works as the Head of Optometry Services for George and Matilda Eyecare.