Pterygia are a common presenting problem in eye clinics in Australia.
The word pterygium derives from the Greek word pteron which means ‘wing’. It has been part of the human ophthalmic experience for many millennia. Early treatments outlined by Celsus, Zarrin-Dast and Ali Inb ‘Isa included excisions with horse’s hair or topical treatments such as licorice, ginseng, burned copper or ammonium salt (Hirst LW. Surv. Ophthal. 48.2 March 2004).
By the time of Serafeddin Sabuncuoglu, however (1385-1468), treatments were marginally more sophisticated. This brilliant surgeon lived in central Anatolia and authored in Turkish, one of the first ever illustrated surgical textbooks on treatments as varied as hydrocephalus and the imperforate anus. The illustration in figure one shows him treating a pterygium. Either his anaesthetic techniques were ahead of his time or the Ottoman patient depicted was very stoic.
Pathogenesis
Whilst ultraviolet exposure is believed to play a significant role in its aetiology, the pathogenesis of pterygium is still poorly understood. There is some epidemiological evidence that suggests that UV exposure in early life is particularly important, perhaps with reflected light impacting on the limbal stem cells nasally, inducing cellular change. Recent studies have suggested that cytokine and various growth factor irregularities may play a role, although the picture is far from complete.
Patients in Australia usually present early with concerns about irritation, cosmesis and less frequently reduced vision. In other parts of the world where eyecare is less available or affordable, the presentation can be much later with significant visual loss
Clinical Presentation
Patients in Australia usually present early with concerns about irritation, cosmesis and less frequently reduced vision. In other parts of the world where eyecare is less available or affordable, the presentation can be much later with significant visual loss. In my trips to Myanmar, with the Myanmar Eye Care Project, pterygium is the most common cause of corneal blindness and pterygium surgery is second only to cataract surgery as the most common procedure performed in the clinics (Figure 1).
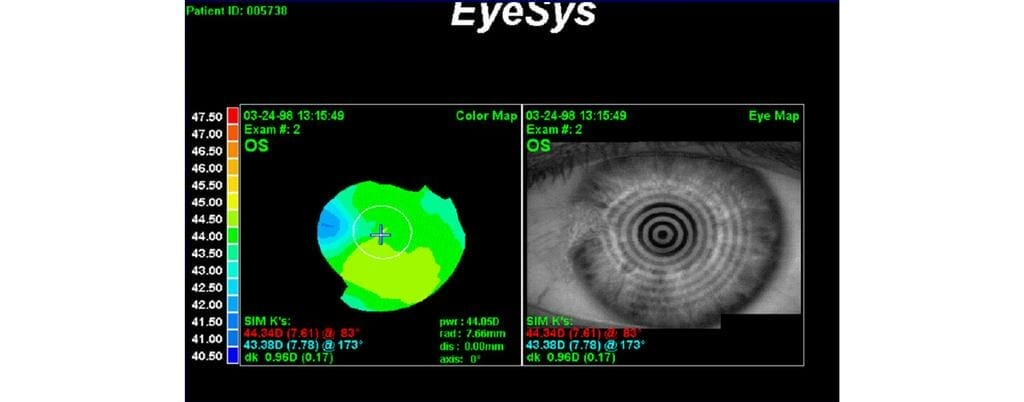
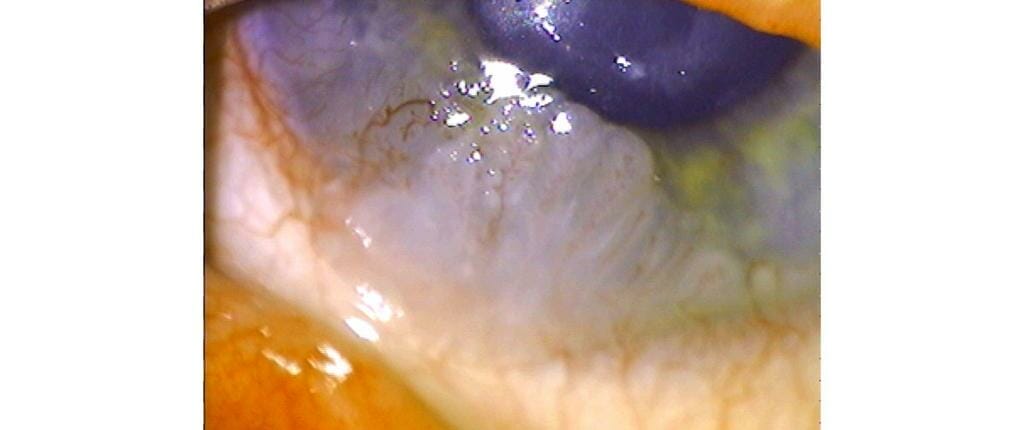
Examination usually reveals a triangular shaped lesion, most commonly at the nasal limbus by definition encroaching on the cornea (Figure 2). There may be various degrees of inflammation, an iron deposition line (Stocker’s line), and some stromal thickening in the advancing head. Before the pterygium gets anywhere near the visual axis, it can induce large amounts of astigmatism (Figure 3).
Differential Diagnosis
The diagnosis is usually very straight forward although there are a few disease processes that can mimic it to some degree. Pingueculae are identical to pterygia pathologically and probably aetiologically, but do not encroach on the limbus. Nor are they triangular in shape. Carcinoma in situ neoplasia can be found at the nasal limbus but again are not triangular and often have a frosted glass appearance (Figure 4). Perhaps the most difficult diagnosis to exclude is in fact a pseudopterygium, which develops as a healing response to trauma or limbal inflammation. Classically with these lesions, a passage for a probe can be found under the neck and the distinction is actually important because they can respond differently to surgical intervention.
Treatment
Prevention of pterygia mandates UV protection in the form of sunglasses and hats (Mackenzie FD et al. ophthal. 99:1056. 1992). This Australian survey suggests that wearing a hat can reduce the incidence by half and sunglasses by nine fold.
In many cases conservative treatment is all that is necessary. Topical lubricants are useful at the first sign of irritation and whilst topical steroids such as fluorometholone are very effective in quietening down the inflammation, their associated side effects of cataract and glaucoma, mandate that they are only used sparingly. Topical vasoconstrictors are commonly used by self medicating patients concerned about cosmesis, but are of little long-term benefit and often counterproductive.
The indications for surgical intervention include visual reduction due to encroachment on the visual axis or more commonly induced astigmatism, excess irritation not controlled by conservative measures and evidence of growth towards the visual axis. Cosmesis, in my opinion, should never be an indication for surgery because of the risk of recurrence. When recurrence does occur it tends to be associated with more inflammation than the primary lesion and correspondingly worse cosmesis!.
The rate of recurrence depends on the technique and type of pterygium and can vary from 15 per cent to less than 1 per cent. In my most recent surgical audit of 150 consecutive pterygia using a conjunctival autografting technique and followed for a mean of 19 months, the recurrence rate was 0.6 per cent. Using a similar technique, Professor Lawrie Hirst, reported at the recent Sydney Eye Hospital: Ophthalmology in the Next Millenium Conference a similar low recurrence rate with follow up to five years (personal communication).
A range of techniques are currently being used for the treatment of pterygia. I use a conjunctival autografting technique with an emphasis on tenon removal and careful wound apposition with fine 10/0 Biosorb sutures which later dissolve. Other techniques include using a sliding conjunctival flap, the use of fibrin glue, amniotic membrane, mitomycin C and even today beta radiation therapy. Whilst there are advocates for all these techniques, there is no evidence that any produce lower recurrence rates that the autografting technique and it remains my procedure of choice, giving an excellent cosmetic result (Figure 5). The alternatives on the other hand have potential drawbacks (scleral necrosis, inferior cosmesis or increased cost) (Figure 6).
I avoid operating on young patients with active ocular inflammation and treat aggressively any inflammation I detect in the postoperative period. One tell-tale sign of an aggressive pterygium that should ring alarm bells and not be operated on unless absolutely necessary, is the presence of small microhaemorrages in the head of the pterygium.
In conclusion, pterygium is like most eye diseases, prevention is better than cure. Careful patient selection and meticulous surgical technique improves outcomes.
Dr Gerard Sutton is a Clinical Associate Professor of Ophthalmogy at Auckland University, Senior Staff Specialist at Sydney Eye Hospital and in private practice at The Eye Institute in Sydney.
His areas of expertise are Corneal, Refractive and Cataract surgery. He has published over 40 peer reviewed papers and textbook chapters. He has pioneered a number of surgical techniques in Australia. He was the first surgeon in NSW to insert an Artificial Cornea and the first surgeon in Australia to use the Intacs intrastromal ring for the treatment of Keratoconus and the first to perform LASIK with the Intralase femtosecond laser. He was also the first surgeon in Australia to perform Penetrating Keratoplasty, Deep Anterior Lamellar Keratoplasty and Descemets Stripping Endokeratoplasty with the femtosecond laser. His research focus continues to be in Corneal and Refractive Surgery with a particular interest in the causes and treatment of Keratoconus.
Gerard has performed and taught cataract and corneal surgery in Cambodia and Burma and remains part of the Myanmar Eye Care Project team. Outside work he is a family man, rugby coach and all too occasionally a flyfisherman.