This is the frst of a two-part series on herpes simplex eye disease.
Herpes simplex eye disease is the most common infection of the cornea, but can affect any part of the ocular structures. This highly prevalent disease affects approximately one third of the world population, with an incidence rate estimated at 8.40 per 100,000 of population per year.
| Take-home Key Points |
|---|
|
The clinical diagnosis of herpes simplex keratitis (HSK) is relatively straight forward when a dendritic corneal ulcer is detected in a patient with an irritated, photophobic red eye. Yet herpes simplex virus (HSV) infection is part of the differential diagnosis of conjunctivitis and keratitis, where clinical features are not always diagnostic.
Humans usually acquire HSV infection early in life. This DNA virus then remains dormant in sensory ganglia. Many initial infections are sub clinical, such as a self-limiting pharyngitis. Follicular conjunctivitis or blepharoconjunctivitis with lid skin vesicles is taught as indicative of an initial contact with the virus or primary infection.
By contrast, corneal disease has always been considered recurrent infection, in a patient who already carries HSV in their ipsilateral trigeminal ganglion.
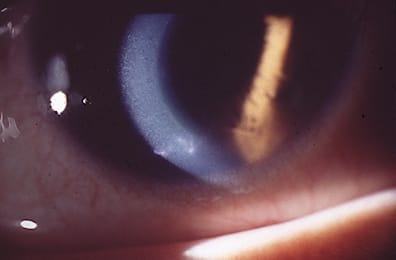
Dendritic corneal ulceration (Image 1), from which HSV DNA is recoverable on polymerase chain reaction (PCR) testing, is found in patients with no clinical history of HSV infection, such as cold sores.
Serology testing will often be positive for anti-HSV IgG antibody in these patients, indicating prior exposure to HSV and production of anti-HSV antibodies in an immunocompetant person. Unilateral or bilateral follicular conjunctivitis with or without epithelial or subepithelial keratitis can also indicate recurrent disease in a patient who has previously suffered a dendritic corneal ulcer.
[/vc_column_text][/vc_column]
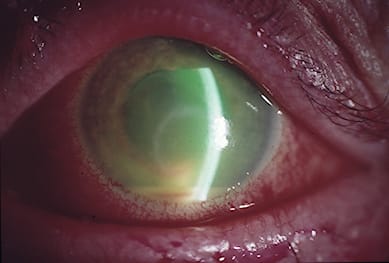
Corneal epithelial HSK can be more difficult to diagnose clinically when it presents as a marginal keratitis (Image 2). Dendritic figures do not retain their characteristic ulcer pattern when located adjacent to the limbus. Their differential diagnoses include ulcerating staphylococcal marginal infiltrate and bacterial keratitis. Early HSK ulcerates first before an infiltrate localises, staphylococcal marginal keratitis does the opposite and bacterial corneal infection is distinguished by significant stromal white blood cell recruitment together with anterior chamber inf lammation.
Herpes simplex keratitis (HSK) can present as corneal stromal or endothelial inf lammation. Stromal inf lammation, either necrotising or non-necrotising, can cause corneal scarring and much less frequently corneal perforation. HSV endotheliitis results in corneal stromal and epithelial oedema (disciform keratitis). HSV should be considered when seeking a cause for a unilateral uveitis. (Image 3)
Host immunity against HSV infection can be compromised by atopy and older age. Patients with severe eczema for example, may present with bilateral keratitis. Trigger factors for epithelial HSK include excess ultraviolet (UV) light exposure, intercurrent illness causing fever and epithelial toxicities such as some topical glaucoma therapies e.g. prostaglandin analogues. These causes of HSK can be under-recognised unless a comprehensive history is obtained from the patient.
The Herpetic Eye Disease (HED) Study has provided evidence-based guidelines for appropriate therapy in HSV eye disease. Conjunctivitis and corneal epithelial disease will heal with topical antiviral (aciclovir ointment), but oral antiviral (famciclovir, valaciclovir and aciclovir) is also excreted in the tears. Oral therapy is an alternative when topical therapy is not tolerated or proves too difficult to administer.
Corneal stromal disease and endotheliitis resolves with topical steroid. Although it is thought to be inf lammatory rather than infective, epithelial HSK can supervene and combined therapy with steroid and antiviral is recommended initially1.
Similarly, presumed HSV iritis is managed with sufficient topical steroid to clear leukocytes from the anterior chamber, together with antiviral cover.
Aciclovir (topical or oral), has remained efficacious in the treatment of human HSV ocular disease and ocular surface toxicity can be managed by reduced dosage once epithelial disease is resolving. Superficial punctuate keratopathy in the inferior cornea is the major sign of such toxicity.
The HED Study confirmed the value of oral aciclovir 400mg twice a day, in reducing the frequency of recurrences of ocular HSV infection, by 40 to 50 per cent. Such treatment does not induce remission. Valaciclovir has significantly better bioavailability (60 per cent) as compared with aciclovir (25 per cent). None of the oral antivirals is funded under the Pharmaceutical Benefits Scheme for treatment of HSV ocular disease.
Therapeutic options for managing HSV ocular infection are expected to increase. Ganciclovir which selectively inhibits HSV DNA has been formulated as a gel, for topical use. New antiviral agents are being developed, including helicase- primase inhibitors,2 preventing viral replication by inhibition of unwinding of viral DNA.
Dr. Kathy McClellan is a Clinical Associate Professor, Discipline of Ophthalmology and Save Sight Institute, University of Sydney; Visiting Medical Offcer Liverpool Hospital & Children’s Hospital at Westmead and Honorary Associate Ophthalmologist Sydney Eye Hospital, specialising in cornea and external eye diseases.
References:
- Wilhelmus K et al., Risk factors for herpes simplex virus epithelial keratitis during treatment of stromal keratitis or iridocyclitis. Herpetic Eye Disease Study Group. Br J Ophthalmol 1996;80:969
- Kaufman HE et al., Efficacy of a helicase-primase inhibitor in animal models of ocular herpes simplex virus type I infection. J Ocul Pharmacol Ther 2008;24:34