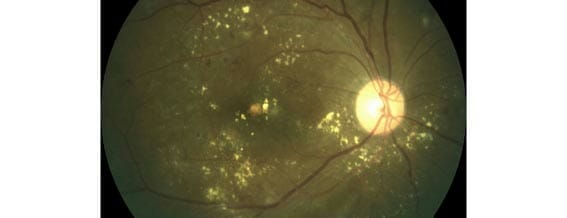
Treatment for diabetic retinopathy has traditionally centred on preventing and slowing disease progression. However, recent studies have revealed new treatments of the disease can improve a patient’s vision.
Diabetic retinopathy is the most common cause of visual impairment and blindness in working adults aged between 20 and 65. Extrapolating from the 10 year incidence of diabetic retinopathy, the risk of diabetic retinopathy is 7–9 per cent per year. The risk of progression to proliferative diabetic retinopathy is 1–3 per cent per year. Because of this, diabetic retinopathy has a very high socio-economic cost.
There are many signs of diabetic retinopathy; microaneurysms, dot and blot hemorrhages, hard exudates, cotton wool spots, intraretinal microvascular abnormalities (IRMAs), venous beading and new vessels. None of these signs are specific for diabetes and can occur in non-diabetic persons as well as with other systemic (e.g., hypertension) and ocular conditions (e.g., vein occlusion, radiation). It is the pattern,symmetry and evolution of these signs that help characterise the appearance of diabetic retinopathy.
Management and Treatment
The management of diabetic retinopathy centers on systemic treatment to prevent the disease from developing and also to lessen its progression. This centres on tight sugar control, management of hypertension and dyslipidemia management.
Intravitreal Lucentis with prompt or deferred focal laser had superior vision and OCT outcomes compared with focal laser treatment alone
The ocular treatment of diabetic retinopathy aims to prevent vision loss and established retinopathy. Without doubt this requires the co-management of diabetic patients between the generalpractitioner,endocrinologist, optometrist and ophthalmologist.
Two visually threatening aspects of the disease are diabetic maculopathy and proliferative diabetic retinopathy. Until recently the mainstay of treatment for both has been laser photocoagulation. While laser photocoagulation has saved the vision of countless diabetics, it has always centered on the prevention of further vision loss. The Diabetic Retinopathy Study (DRS) was published 30 years ago. The aim was to evaluate if retinal laser photocoagulation could reduce vision loss in patients with proliferative diabetic retinopathy. The results showed that laser photocoagulation reduced the rate of severe vision loss by 50 per cent (Severe vision loss was defined by vision of less than 5/200 on the Snellen equivalent chart).
The Early Treatment of Diabetic Retinopathy Study (ETDRS) investigated the role grid laser treatment played in the management of Diabetic Macular Edema (DME). The results were promising and revealed that grid laser treatment of DME reduced the rate of moderate vision loss by half at three years. (Moderate vision loss was defined as a doubling of the visual angle, the loss of 15 letters or more on the Snellen equivalent chart).
Even the mechanism of laser in preventing vision loss is debatable. It is argued that laser photocoagulation induces the destruction of oxygen consuming photoreceptors. Once this happens oxygen can diffuse from the underlying choriocapillaris, through the resultant microscopic scar to the inner retina. This then relieves the relative hypoxia in the inner retina. Alternative theories include the potential for laser to aid in the restoration of a new retinal pigment epithelial barrier (RPE). The RPE responds to injury in a number of ways; firstly, if the defect is small, the RPE cells spread to cover the defect (<125µm). If the defect is large, laser photocoagulation can result in RPE cell proliferation to resurface the defect area. This new RPE layer can then produce cytokines that can antagonise the permeabilising effects of Vascular Endothelial Growth Factor (VEGF), reducing the intraretinal swelling that is the hallmark of DME.
While both the DRS and ETDRS were landmark studies and have laid the foundation of diabetic retinopathy management for the 30 years that followed, the outcomes we have been aiming for are the prevention of moderate and severe vision loss as defined by these studies.
Promising New Treatments
It is very promising that some recent studies have shed light on some very promising new treatments for Diabetic Macular Edema (DME) in particular.
The RESOLVE, RESTORE and DRCR.net DME studies have all been investigating the role of Lucentis (Ranibizumab) in the management of DME. Better known for its role in the treatment of neovascular macular degeneration, Lucentis appears to have a role to play in treating visually threatening diabetic retinopathy.
The RESOLVE study revealed Lucentis treated patients showed clinical and statistical superiority versus sham for improvements in vision and central retinal thickness on OCT scanning. Importantly, the safety profile of Lucentis in patients with DME was similar to that reported in patients with macular degeneration.
In the RESTORE trial, intravitreal Lucentis alone, or as adjunctive therapy to laser photocoagulation, provided superior benefits in vision improvement as compared to laser treatment alone. This study shows that 37-43 per cent of Lucentis treated patients improved vision by 10 letters or more as compared to 16 per cent with standard laser therapy.
The DRCR.net trial also showed intravitreal Lucentis with prompt or deferred focal laser had superior vision and OCT outcomes compared with focal laser treatment alone. Here 50 per cent of eyes had substantial improvement by 10 letters or more, while ~30 per cent gained greater than 15 letters. This study also looked at the efficacy of intravitreal steroid injections for DME. In pseudophakic eyes, intravitreal triamcinolone with prompt focal laser may be equally effective as Lucentis at improving visual acuity and reducing retinal thickening, but is associated with an increased risk of intraocular pressure elevation.
The most amazing component of these results is the sheer number of patients whose vision improved with treatment for their diabetic maculopathy. In the not too recent past, the sole aim in treating diabetic eye disease was to simply stabilise vision and prevent further vision loss. The results of this study are analogous to the landmark studies involving Lucentis outcomes in wet macular degeneration.
Applications are currently being made to the federal government to have intravitreal Lucentis approved for use in diabetic macular edema in Australia. While this is pending Avastin (Bevacizumab), a closely related drug, is being used as a substitute.
Dr. Timothy Nolan is a Medical Retina Specialist who practices exclusively in the treatment of diseases involving the macular and retina. He lectures in the Department of Ophthalmology at the University of Sydney, has published a number of articles in the scientific press and is the Director – Retina Associates at Eastern Suburbs Retina and South West Retina.