This month we review new models to measure patient outcomes, the value of surgical experience and new technologies that will to enhance the process of cataract surgery.
Over three years, data on outcomes from cataract and refractive surgery from around the world has been collected and it’s now contributing significantly to improvements in treatments and standards of care. The project, cofounded by the European Union and the European Society of Cataract and Refractive Surgeons, has resulted in a database containing data on 820,000 cataract surgeries.
Data on 368,256 cataract extractions reported to the European Registry of Quality Outcomes for Cataract and Refractive Surgery database has been analysed to determine visual outcome after cataract surgery.
The study, published in Cataract Refractive Surgery1 found that the best visual outcome was achieved in age groups 40 to 74 years, and that men showed a higher percentage of excellent vision (1.0 [6/6] or better) than women. A corrected distance visual acuity (CDVA) of 0.5 (6/12) or better and of 1.0 (6/6) or better was achieved in 94.3 per cent and 61.3 per cent of cases, respectively.
Data on 368,256 cataract extractions reported to the European Registry of Quality Outcomes for Cataract and Refractive Surgery database has been analysed to determine visual outcome after cataract surgery
The authors notes that, “the visual outcomes of cataract surgery were excellent, with 61.3 per cent of patients achieving a corrected distance visual acuity of 1.0 (6/6) or better. Age and sex influenced the visual outcomes, but the greatest influences were short-term postoperative complications, ocular comorbidity, surgical complications, and complex surgery. A weakness of the study could be that some of the data is self-reported to the registry.”
Comment
Dr. Joe Reich
It should be noted that 26 per cent of patients had an ocular co-morbidity and 12 per cent required ‘complex’ surgery. Not surprisingly the poorest outcomes occurred with known preoperative macular degeneration and amblyopia yet most had improved vision after surgery. An important finding was the fact that patients with diabetic retinopathy and other co-morbidities had a significant risk of loss of best vision. (See Figure 1 page 39)
Correcting Surgical Presbyopia
Patients can now expect to enjoy good unaided distance visual acuity following cataract surgery and intraocular lens (IOL) implantation. Near vision, however, still requires additional refractive power,
usually in the form of reading glasses. A 2012 Cochrane Review2 assessed the effects of multifocal IOLs, including effects on visual acuity, subjective visual satisfaction, spectacle dependence, glare and contrast sensitivity, compared to standard monofocal lenses in people undergoing cataract surgery.
Multifocal IOLs are more effective at improving near vision relative to monofocal IOLs. Adverse subjective visual phenomena, particularly haloes, or rings around lights, and evidence of reduced contrast sensitivity were more prevalent and more troublesome with the multifocal IOL. Whether that improvement outweighs the adverse effects of multifocal IOLs will vary between patients and motivation to achieve spectacle independence is likelyto be the deciding factor.
Comment
Dr. Joe Reich
Multifocal lenses are best used where there are no significant ocular comorbidities, in patients where emmetropia can reasonably be achieved and where the limitations of the technology are understood by the patient. As indicated motivation for spectacle freedom is important.
Correcting Myopia
In another study,3 researchers compared correction for moderate to high myopia with phakic intraocular lenses (IOLs) vs. excimer laser refractive surgery. Phakic IOLs can be placed either in the anterior chamber in front of the iris or in the posterior chamber between the iris and the natural lens.
Excimer involves reshaping the corneal stroma to alter the refractive power of the cornea and bring the image of a viewed object into focus onto the retina.
The report suggests that phakic IOLs are safer than excimer laser surgical correction for moderate to high myopia in the range of -6.0 to -20.0 D and that phakic IOLs are preferred by patients.
The authors noted that “while phakic IOLs might be accepted clinical practice for higher levels of myopia (greater than or equal to 7.0 D of myopic spherical equivalent with or without astigmatism), it may be worth considering phakic IOL treatment over excimer laser correction for more moderate levels of myopia (less than or equal to 7.0 D of myopic spherical equivalent with or without astigmatism)”. They noted that further research is required.
Comment
Dr. Joe Reich
Phakic IOL use may well be the better choice when corneal refractive surgery is contraindicated (higher myopia, thin cornea, corneal irregularities) but have their own limitations. They do have a higher (though often not significant) risk of reduction in corneal endothelial cell density, induced cataract and the risks of intraocular surgery.
Correcting Residual Refractive Error
In a retrospective multicentre study published in The Journal of Refractive Surgery4 the efficacy, predictability, and safety of intraocular lens (IOL) exchange in comparison with piggyback lens implantation and LASIK to correct residual refractive error following cataract surgery was evaluated.
The authors of ‘Resolving refractive error after cataract surgery: IOL exchange, piggyback lens, or LASIK’, found that while all three procedures were effective, the Lasik group showed the best outcomes in efficacy and predictability.
Comment
Dr. Joe Reich
While all were reported to be similar in outcome, it is important to note the difficulty of IOL exchange if YAG
laser capsulotomy has been undertaken, and the difficulty of reimplanting a toric lens in such a situation. Also with capsule fibrosis, late term lens exchange is more difficult.
Piggy back lenses may correct ammetropia but are relatively crude at correcting astigmatism. The study validates the use of refractive laser as the least invasive technique. Surface laser treatment is also advocated rather than LASIK due to the excellent visual outcomes achieved with what are usually low refractive errors. (See Figure 2)
Comment
Dr. Tim Roberts
Good refractive outcomes begin with a good understanding of the patient’s visual goals – what does your patient really want and what is your patient really expecting – and knowing what refractive outcomes you can confidently expect from your surgery. Careful patient selection and pre-operative counselling, combined with accurate biometry, results in realistic expectations and a high level of satisfaction.
Educating patients about the expected post-operative experience with a multifocal IOL differs from individual to individual. Avoiding the term ‘multifocal’ is advisable in those who were unable to adapt to multifocal spectacles. Using a multifocal contact lens in those with reasonable vision (usually refractive lens exchange cases) is an option, however the results are variable and often underwhelming. Web-based simulators viewed on a PC or tablet can be helpful for some to experience the difference.
Proper patient selection and education remain the most important factors – patients need to be motivated and desire uncorrected reading vision as the primary outcome, rather than a bonus. These patients have the best chance of adapting and accepting that any night glare and loss of contrast are an acceptable compromise, and well worth the gain in uncorrected near vision.
Value of Surgical Experience Measured
Cataract surgery forms a core part of every ophthalmologist’s training. However, it is the experience of the surgeon, the understanding and analysis of their surgical outcomes, and ability to understand patient need that plays a key part in achieving the best patient outcome. Several studies have recently been published into the impact that experience has on patient outcomes and to a great extent they concur that despite a steep learning curve, outcomes for surgeons appear to be similar once they have performed 100 cataract surgeries.
Comment
Dr. Joe Reich
The range of published complication rates for cataract surgery are quite variable and often disturbingly high, especially with critical complication such as capsule tears, vitreous loss and dropped nuclei which are known to reduce post-surgical visual outcome.
The study of 368,256 commented upon earlier, identified that these complications occurred in three of every 200 cases. The recent large study of LenSx cases in Sydney shows a much lower rate of these significant complications.
So while there may be some similarity of outcomes in those with a hundred cases, the published data of high volume cataract surgeons shows significant reductions in surgical risk with experience and volume.
Benefits of Bilateral Cataract Surgery Highlighted
Same-day, or immediately sequential, bilateral cataract surgery (ISBCS) is being practised with increasing frequency worldwide.
In a study published in Survey of Ophthalmology (November 2012),5,6 the authors of Same-day cataract surgery should be the standard of care for patients with bilateral visually significant cataract wrote that ISBCS “provides many advantages including convenience for the patient and the patient’s family”, because it repairs the visual system (not just one eye) and restores normal binocularity as well as unilateral clarity. Additionally, they wrote, ISBCS “creates a much more relaxed surgical atmosphere in harried operating rooms, and saves money for society. It is often preferred by busy professionals”.
The study identified numerous benefits for sequential surgery that included the ability to assess the outcome of the first surgery then tailor the surgical technique, intraocular lens (IOL) power, and choice of IOL for the second surgery. Additionally, they found, recovery may be prolonged from corneal edema, anterior chamber inflammation, or cystoid macular edema.
“Allowing the patient to maintain visual function in one eye during the recovery of the other eye can be important. Therefore, the few benefits of simultaneous surgery are greatly outweighed by risks of bilateral complications, inability to foresee refractive outcome, inability to alter IOL choice, potential loss of physician reimbursement, and possible increased legal ramifications,” they wrote.
The authors claimed that the purported risks of ISBCS had not been supported by the literature. Those risks included bilateral retinal detachment, bilateral corneal decompensation, bilateral diabetic macular edema, bilateral severe cystoid macular edema, significant IOL power errors in the first eye that could be refined and thereby prevented in the second eye, and toxic anterior segment syndrome.
“The greatest fear of ISBCS has been possible simultaneous bilateral endophthalmitis, which did not occur in a series of nearly 100,000 ISBCS cases and has only occurred elsewhere when complete separation of the two eyes and strict sterile protocol were not followed The International Society of Bilateral Cataract Surgeons (www.isbcs.org) has prepared the ‘ISBCS General Principles for Excellence in ISBCS’, which should be followed for safe ISBCS.”
Comment
Dr. Joe Reich
While there were no reported cases of endophthalmitis in the series of 100,000 cases the editor is aware of cases in Australia. Simultaneous surgery may benefit some patients travelling long distances but the risks of bilateral complications, problems with IOL powers and the fact that in Australia Medicare will pay only a 50 per cent benefit for second procedure during the one operating room admission make this a costly exercise as well.
Pre- and Post-operative Care
Routine pre-operative medical testing has not been found to increase the safety of cataract surgery, according to a study published in the 2012 Cochrane Review.7 The authors instead proposed that in developed countries, alternatives including self-administered health questionnaires may lead to cost-effective means of identifying those at increased risk of medical adverse events due to cataract surgery.
The authors, who reviewed three randomised clinical trials wrote, “most cataracts are performed on older individuals with correspondingly high systemic and ocular comorbidities. It is likely that routine preoperative medical testing will detect medical conditions, but it is questionable whether these conditions should preclude individuals from cataract surgery or change their perioperative management”.
Despite the rare occurrence of adverse medical events precipitated by cataract surgery, they said the issue remains a concern because of the large number of elderly cataract patients with multiple medical comorbidities.
The cost of cataract surgeries including preoperative medical testing was found to be 2.55 times higher than cataract surgeries without preoperative medical testing. There was no difference in cancellation of surgery between those with preoperative medical testing and those with no or limited preoperative testing.
Comment
Dr. Joe Reich
With modern cataract surgery and associated improvements in anaesthesia preoperative health assessment is unnecessary. Consideration may have to be given to diabetic patients where fasting may interfere with their daily routine. Most surgeons will not vary anticoagulant use with planned clear corneal surgery.
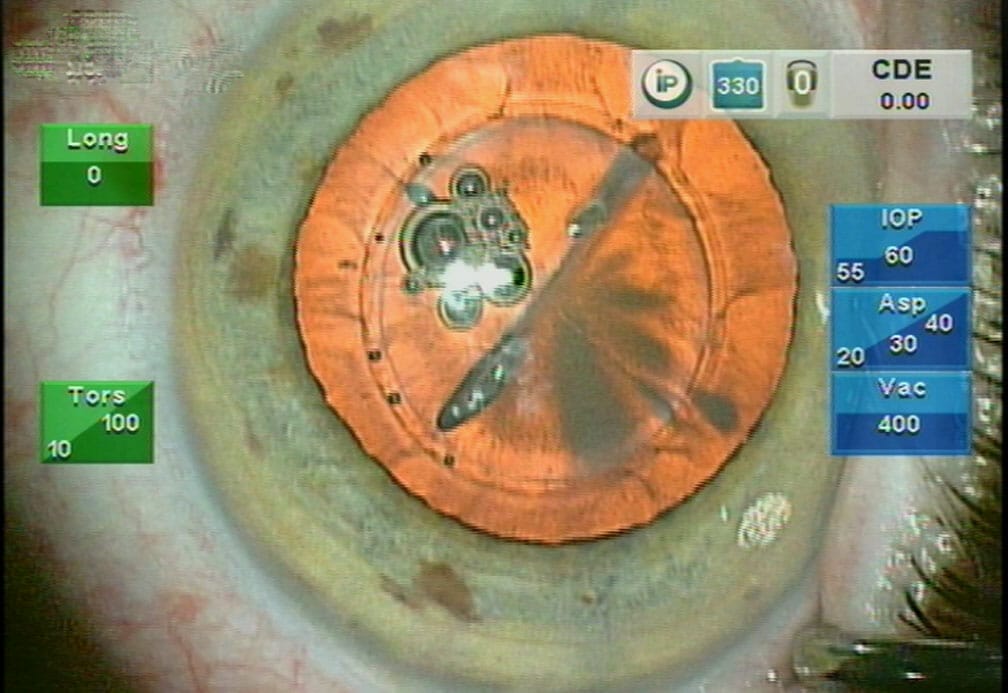
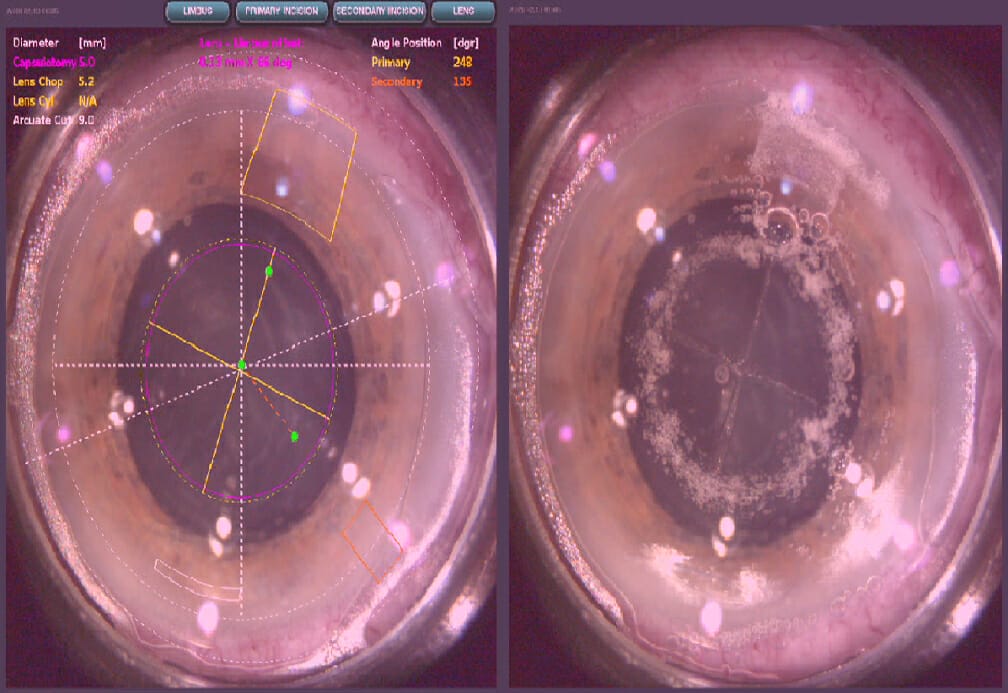
New Sequential Wavefront Device
An important new sequential wavefront device with rapid sampling will help optimise cataract surgery outcomes, according to research published in Journal of Refractive Surgery.8 The study entitled ‘Comparison of IOL power calculation methods and intraoperative wavefront aberrometer in eyes after refractive surgery’, found the “device can be used as an intraoperative, real-time aberrometer/refractometer for immediate diagnosis and management of refractive outcomes during cataract surgery”.
The prototype wavefront device was miniaturised into a narrow profile attachment that can be fixed to an operating microscope.
Researchers noted that the clinical application of the wavefront device was “easily implemented without changing or limiting the working distance, magnification, or illumination of the surgeon’s ergonomics intraoperatively. The real-time wavefront outcome was visualised overlaying a live eye image, presenting the refractive error both qualitatively and quantitatively”.
They predicted that as the precision and accuracy of intraoperative documentation and refinement of outcomes is enhanced the wavefront device would become “an important future tool for optimising cataract surgery outcomes”. (See Figure 3)
Comment
Dr. Joe Reich
The use of intraoperative wavefront analysis is driven by attempting to optimise the visual outcomes in patients whose prior laser refractive surgery makes routine IOL power estimation difficult. However IOL formulae still offer the advantage of simplicity, especially when prior data is available i.e. pre laser K readings.
Wavefront analysis may in the future have a place in aligning a toric lens at the time of cataract surgery. The devices will not be as practical for measuring lens power as any lens power alteration will require a lens exchange during surgery with its attendant risks. In practical terms the ability to undertake adjustment with refractive laser post lens surgery remains a practical, if rarely needed, option.
Comment
Dr. Tim Roberts
Cataract surgery is good, but we can, and must, aim for better results.
What can we improve?
- Better understanding of patient expectations
- Better biometry and IOL calculations
- More accurate and predictable surgery
- Safer surgery
- Better and more accurate refractive outcomes
References
1. Lundström M, Barry P, Henry Y, Rosen P, Stenevi U. Visual outcome of cataract surgery; study from the European Registry of Quality Outcomes for Cataract and Refractive Surgery. Journal Cataract Refract Surg. 2013 May;39(5):673-9. doi: 10.1016/j.jcrs.2012.11.026.
Epub 2013 Mar 14.
2. Calladine D, Evans JR, Shah S, LeylandM. Multifocal versus monofocal intraocular lenses after cataract extraction. Cochrane Database of Systematic Reviews 2012, Issue 9. Art. No.: CD003169. doi: 10.1002/14651858.CD003169.pub3.
3. Barsam A, Allan BD. Excimer laser refractive surgery versus phakic intraocular lenses for the correction of moderate to high myopia. Cochrane Database Syst Rev. 2012 Jan 18;1:CD007679. doi: 10.1002/14651858.CD007679.pub3.
4. Fernández-Buenaga R, Alió JL, Pérez Ardoy AL, Quesada AL, Pinilla-Cortés L, Barraquer RI. Resolving refractive error after cataract surgery: IOL exchange, piggyback lens, or LASIK. J Refract Surg. 2013 Oct;29(10):676-83. doi: 10.3928/1081597X-20130826-01. Epub 2013 Sep 2.
5. Henderson BA, Schneider J. Same-day cataract surgery should not be the standard of care for patients with bilateral visually significant cataract. Surv Ophthalmol. 2012 Nov;57(6):580-3. doi: 10.1016/j.survophthal.2012.05.001. Epub 2012 Sep 18.
6. Arshinoff SA. Same-day cataract surgery should be the standard of care for patients with bilateral visually significant cataract. Surv Ophthalmol. 2012 Nov;57(6):574-9. doi: 10.1016/j.survophthal.2012.05.002. Epub 2012 Sep 18.
7. Keay L, Lindsley K, Tielsch J, Katz J, Schein O. Routine preoperative medical testing for cataract surgery. Cochrane Database Syst Rev. 2012 Mar 14;3:CD007293. doi: 10.1002/14651858.CD007293.pub3.
8. Canto AP, Chhadva P, Cabot F, Galor A, Yoo SH, Vaddavalli PK, Culbertson WW. Comparison of IOL power calculation methods and intraoperative wavefront aberrometer in eyes after refractive surgery. J Refract Surg. 2013 Jul;29(7):484-9. doi: 10.3928/1081597X-20130617-07.
9. Lundstrom M, Barry P, Henry Y, et al. Evidence-based guidelines for cataract surgery: guidelines based on data in the European Registry of Quality Outcomes for Cataract and Refractive Surgery database. J Cataract Refract Surg;38:1086–93.
10. Roberts, Lawless, Sutton et al. Surgical Outcomes and Safety of Femtosecond Laser Cataract Surgery: A Prospective Study of 1500 Consecutive Cases. Ophthalmology 2013;120(2):227-233