On many occasions during his personal journey of retinopexy, cryopexy, vitrectomy and IOL surgery, Professor Nathan Efron found that he had to get by using one eye only… That made him realise the beauty of (normally) having two eyes.
For the benefit of those reading this blog who are not ophthalmic practitioners, ‘stereopsis’ refers to the process by which our two eyes and brain work together to create the perception of a three-dimensional world. Perhaps the best illustration of this phenomenon is when we go to the cinema to watch a 3D movie. The amazing 3D depth sequences, which are essentially exaggerated stereopsis effects, suddenly cease to occur when you cover one eye, or remove your special 3D glasses.
The essence of stereopsis is that you need two healthy eyes with reasonably good vision to be working together to create a three dimensional stereoscopic world. This is the basis of clinical tests of stereopsis, such as the Titmus Stereotest. Reduced or absent stereopsis, as revealed by such tests, indicates a defect in binocular vision.
The problem I am having during various phases of my eye surgery is that, for extended periods, I only have the effective use of one eye. For example, following the initial vitrectomy in my right eye, which subsequently filled with blood, I was essentially blind in that eye for almost two weeks. After I had the revision surgery, it took another two weeks before vision in that eye returned to near normality. During these periods, I was deprived of stereopsis!
Ever tried shaving with one eye? I don’t recommend it! I ended up with a couple of small cuts around my lips and nose
So what’s the big deal about that, you ask? And maybe that is not an unreasonable question. Many people in this world have only one eye, because the other is blind, or has been removed due to congenital abnormality, disease or accident. They can function perfectly well with only one eye. Many of us have been forced to use one eye for brief periods when the other eye is incapacitated due to injury or a severe eye infection.
Of course, the world still looks three-dimensional when you use only one eye, but this is not because of stereopsis. Many other factors are involved. First, you know the world has depth from experience. Second, there are numerous so-called ‘monocular cues’ that signal depth, such as relative size, interposition of objects, linear perspective, aerial perspective, light and shade and monocular motion parallax.
So why should I complain about being deprived of the use of one eye for a limited period? Well, I guess the point is that I am not so much ‘complaining’, as coming to the realisation that stereopsis is a useful attribute. I remember my undergraduate lectures in visual physiology, where we explored the concept and neural basis of stereopsis in great detail. In practical classes we would conduct experiments to demonstrate stereopsis and investigate the visual conditions under which it becomes apparent. As it turns out, stereopsis takes effect at distances of up to 18m away.
In my last blog I discussed my frustration with the practical and logistical difficulties in using eye drops and ointments (using both eyes), and conveyed the sentiment that we ought to have empathy with our patients to whom we prescribe these treatments. Well, the same applies for our patients who are about to become monocular for a period of time. A few words of encouragement, and advice to take care when doing things up close that require judgement of distances, would not go astray. Let me illustrate this with personal experiences during my many surgically-induced monocular phases. There have been various incidents, albeit relatively inconsequential in the big picture of life, of being flummoxed by the absence of stereopsis.
Trouble in the Kitchen
The morning after my first vitrectomy, when I sat down at the breakfast table and proceeded to pour milk into my cereal bowl, I couldn’t be sure exactly where I was pouring the milk, and how high the milk bottle was from the bowl. I had to grab the bowl so as to provide additional orientation cues, relating to where my two hands were with respect to each other. No real problem, but I found myself having to proceed a little more carefully than usual.
Again in the kitchen – our cappuccino maker requires water to be poured into the narrow neck of the boiler. You guessed it… water everywhere except in the boiler the first time I tried to do this (Figure 1A). I developed a strategy of resting the lip of my water jug against the neck of the boiler to ensure accurate pouring.
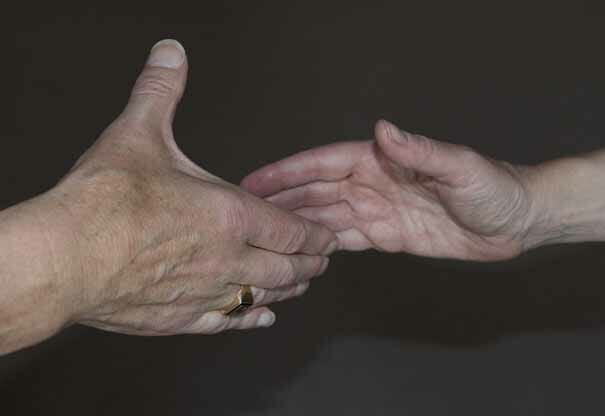
As a well brought up individual, I was accustomed to greeting Bill with a handshake at the beginning of each of my consultations. When I went to shake Bill’s hand following my vitrectomy, I missed making the hand connection (Figure 1B).
It happened momentarily, and only required a slight readjustment to complete the hand shake. I am sure Bill didn’t even notice that this occurred, but it was nevertheless slightly unnerving for me.
Having Type 2 diabetes, I check my blood sugar levels every Sunday morning. This has become a challenge with only one eye. Blood sugar monitoring requires pricking the tip of my finger with a fine lancet and allowing a small droplet of blood to form. Then the end of a 3cm long plastic sensor strip must be dipped into the blood droplet for a few seconds until the blood sugar level readout appears on the digital monitor into which the other end of the sensor strip is inserted (Figure 1C). I found this extremely difficult, as I couldn’t tell if I was approaching the blood drop too high or low, and ended up smearing blood all over the place. Again, no great drama, but a reminder of my lack of stereopsis.
Using the touch screen on my iPhone became quite awkward. Try it yourself after covering one eye. The difficulty is created by not knowing how far your finger is from the touch pad. If the screen is at a slight angle to the line of view, then sometimes the tap target is missed (Figure 1D). In frustration I sometimes resorted to using Siri (automated voice recognition software on the iPhone) to assist with such tasks.
Ever tried shaving with one eye? I don’t recommend it! I ended up with a couple
of small cuts around my lips and nose due to an impaired ability to accurately place the razor on the desired part of my face. Very frustrating. If you don’t believe me, don an eye patch next time you have a shave and see how you fare!
Of more immediate relevance to my eye problems is the instillation of eye drops and ointments, which I find even more difficult with the use of only one eye. The problem is especially acute with the application of ointments because I am unsure of the distance of the tip of the ointment tube’s nozzle from the rim of my lower eyelid. I know it is important not to touch the nozzle against my eye to avoid contamination, but I ended up repeatedly touching my eye by accident.
The Frustration of Monocularity
Perhaps this may have been a better title for this blog, because there are more disadvantages that come with being deprived of the use of one eye than the mere absence of stereopsis. I am referring here to the restricted field of view.
In the immediate aftermath of my right eye vitrectomy, I had a restricted view of everything out to my right hand side (with my head in a fixed position and gazing straight ahead). Of course, this deficit could be overcome simply by rotating my head to the right, and to a lesser extent by moving my eyeball about to extreme positions of gaze, but this is unnatural behaviour. On many occasions during this period I was consciously aware of executing an exaggerated turn of my head to the right to see what was happening on that side.
Taking Things for Granted
Back in optometry school one of my classmates had only one eye. She used to despair during our stereopsis practical classes at being unable to appreciate or really understand what stereopsis means. I remember being a little bemused by this and shrugging off her concerns, but it is only now – after having been forced to cope with one eye for days and weeks at a time as a result of my eye surgeries – that I have developed a healthy respect for the fascinating and most useful physiological trait that is stereopsis.
Professor Nathan Efron is a researcher at the Institute of Health and Biomedical Innovation and School of Optometry and Vision Science, Queensland University of Technology. He is currently president of the Australian College of Optometry and vice-president of the International Society for Contact Lens Research.