Back in the mid-1950s, optometrist Professor Josef Lederer designed aberration controlled spectacle magnifiers and trialled them successfully on 550 of his low vision patients. His study was published in the prestigious journal Nature. Then, in 1974, Professor Ian Bailey was awarded a NHMRC two-year grant to study ‘Vision in Senile Macular Degeneration’. Together with his then graduate student, now Prof. Jan Lovie-Kitchen, he developed the logMAR designation of distance visual acuity with its improved sensitivity gained from letter-by-letter scoring.
Over the years logMAR principles have been adopted by major clinical research studies and are now used in low vision clinics worldwide. They are the hallmark of the ETDRS standard of visual acuity testing, essential for monitoring the efficacy of intra-vitreal anti-VEGF injections.
Just as importantly are the Bailey-Lovie near visual acuity word reading charts that demonstrate the inter-relationship between reading distance, dioptric power of a near spectacle lens, print size in points or M units and image enlargement ratio or magnification. The needed near magnification for a specific reading task is predictable and certain in its benefits.
Contrast… until recently was not greatly influenced by optical means other than selective tints to improve colour separation.
The first agency low vision clinic in Victoria was established in the 1970s, instigated by ophthalmologist Professor Gerard Crock; a collaborative effort between Crock, optometry Professor Barry Cole and John Wilson, director of the Association for the Blind at Kooyong, Victoria, now Vision Australia.
Former ophthalmic nurse and Churchill Fellowship awardee Margaret Biggs managed the Kooyong low vision clinic, showing an unforgettable charisma and empathy for her patients and clinic staff. With its curious name and under Margaret’s guidance, the clinic became the jewel in the crown of the Association, attracting visitors from all over the world to observe its multi-disciplinary care model where, for the first time in Australia, ophthalmologists and optometrists consulted together.
Those were halcyon days with generous funding from a Whitlam government Health Program Grant. The Association for the Blind hosted international low vision conferences in 1980 and 1990; events that were to become the forerunners of the triennial International Low Vision Conference held in different cities around the world.
Rehabilitation Care
University optometry clinics and agency low vision clinics continue to provide a breadth of rehabilitation care, integrating a multidisciplinary approach with the inclusion of orthoptic expertise, occupational therapy, mobility advice, social welfare and vocational training.
Special liaison with primary and secondary educational services for vision-impaired children offers lifelong benefit; opportunities that were less readily available in the past.
Our increasing and aging population means that more people than ever face the scourge of macular degeneration, despite the miracle of anti-VEGF treatment. Maintaining independent living for our elders is cost effective, in terms of both ability to perform activities of daily living and to enjoy a good quality of life.
Since those late 20th Century years, optometric education has changed to adapt to a more shared-care model with ophthalmology, with greater emphasis on disease detection and treatment using some therapeutic drugs. Some loss of emphasis on refraction, low vision optics and spectacle dispensing in teaching programs means that students may gain less experience in low vision as a sub-set of optometric skills. The prescription of excellent bioptic telescopes and high power near magnification of the Lederer type, but in modern aspheric acrylic lens form, is not high on the list of expertise that a graduating ophthalmic student possesses.
An awareness of rehabilitation needs in older patients is still essential. In a remarkable study published in The Lancet in September 2015, the global burden of disease (GBD) was analysed for 306 diseases in 186 countries.1 From these data, disability adjusted life years (DALYs) were calculated from the sum of years lived with disease (YLD) and years of life lost (YLL) due to early death. These data vary by country and are inexact (up to ±10 per cent or so) but give a fair view of global health. From 2005 to 2013 the world’s population increased by 9 per cent but its total DALYs per 100,000 of population fell substantially, by 25 per cent for communicable diseases and about 6 per cent for non-communicable diseases.
DALYs for cataract, glaucoma and all other diseases decreased by between 5 and 9 per cent, but those for macular degeneration increased by about 10 per cent, a reflection of our global increasing longevity. Interestingly, DALYs for uncorrected refractive error were about 75 per cent more than DALYs for all eye conditions, reinforcing the need to address this concern that limits educational and economic progress particularly in developing countries. The US National Institutes of Health National Eye Institute (NEI) acknowledges that the overall number of DALYs per 100,000 of population for eye disease is small, but patients disabled by eye disease require whole-of-life rehabilitation care, placing vision impairment amongst the 10 most prevalent causes of disability in the United States. The NEI recommends that a broad-based program is necessary to educate clinicians, neuroscientists, and engineers from a variety of backgrounds about the research opportunities in low vision and blindness rehabilitation.
New Technologies Taking Favour
We understand low vision optics well. Major clinics have a large variety of well-designed, illuminated aspheric magnifiers, and complex high power bifocal and diffractive optics are commercially available for speciality prescriptions. We have Galilean and Keplerian telescopes in many options, and know that widest fields of view are obtained from through-the-lens bioptic Keplerian systems rather than in-front-of-the-spectacle-lens Galilean systems that often disappoint. We know that the patient with an essential vocational need appreciates the value of these expensive devices and understands that device cost is amortised against convenience over 10 or more years, making affordability more understandable.
We also understand the recent technological revolution that is the smartphone, an invention now as ubiquitous as the scissors, Band-Aid and plastic wrap. This is the device that reputedly has more computing power than the computer of Columbia’s Eagle, the 1969 lunar lander. It is universally available in every country – just observe commuters on public transport or in an airport lounge. Recently when I asked a 20-something patient with albinism whether she still used her 6x monocular telescope, she replied “nope, no street cred!” preferring to capture a smartphone image of a bus number and zoom up magnification, an event that is universally ignored as commonplace.
Our low vision clinics must adapt to this technological revolution. There is still a need for closed circuit TV magnification and more complex magnification options in school and workplace settings. However, the potential of the smartphone is barely tapped. It can be used for mobility support with GPS technology, it offers speech recognition and has optical character recognition (OCR) text-to-speech output. Simple low-cost apps (<$10) provide magnification with contrast reversal and enhancement, ideal for shopping tasks or restaurant menus. In the immediate future, expect speech recognition and instant translation, making the China visit less of an uncertainty when supportive bilingual Chinese colleagues are not at hand. It is certain that our low vision patients of tomorrow will rely less on optical enhancement and more on alternative senses such as hearing and speech. The magnifying glass has a challenger, but is not written off!
Importance of Contrast
Finally, let me mention the importance of contrast. Illumination engineers consider contrast to be the key to visibility, whereas ophthalmic practitioners stress acuity in the first instance. In fact, both image features are essential. We know that greater task illumination improves visibility, but does so by increasing retinal gain rather than by changing contrast. Contrast is principally a feature of the colour and texture (reflectance) of objects, and until recently was not greatly influenced by optical means other than selective tints
to improve colour separation.
US optometric researcher Dr. Eli Peli from the Schepens Eye Institute of Harvard University has developed an augmented visibility application that outlines faint contrast borders in a head up display in real time. The potential for improved visibility is exciting. What is the more remarkable is this technology readily adapts to smartphone use. Figure 1 shows the smartphone used as a virtual reality display on a vrAse headset, presenting stereo images binocularly from a split screen display.
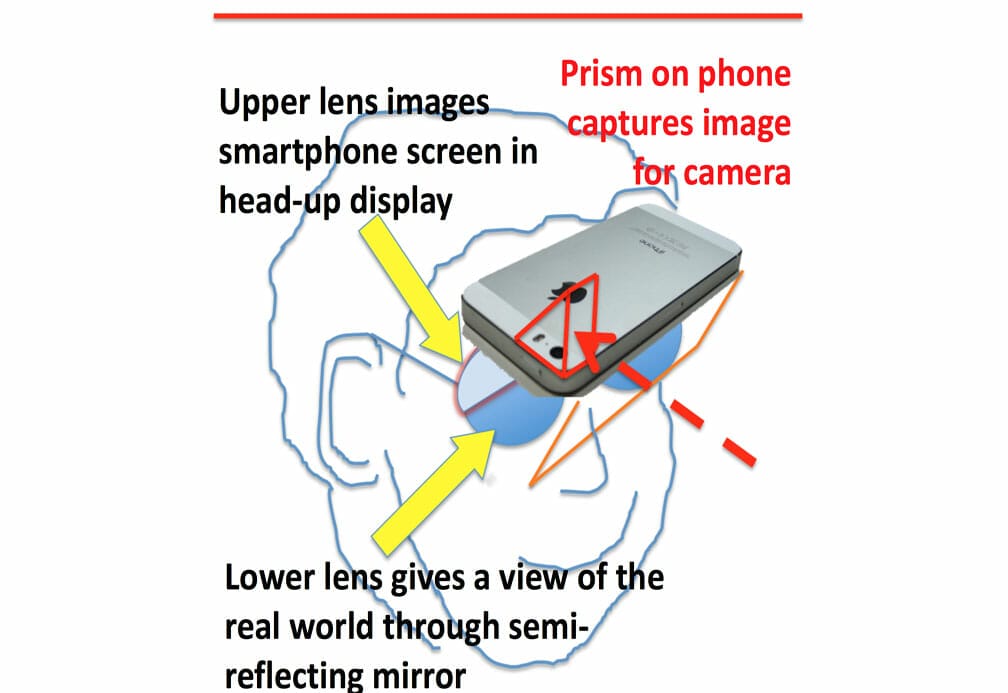
It is little stretch of the imagination to see how a smartphone can be mounted horizontally and imaged through a semi-reflective screen mounted at 45 degrees to the line of sight. In the upper segment of a spectacle lens we use a collimator to image the screen, while the lower segment views the real world through any needed ametropia correction. A suitable prism over the camera optics reflects the scene into the camera for magnification, image reversal or contrast enhancement as needed. Smartphone software for image orientation and alignment is already available and all that is needed is a Bluetooth earpiece and microphone controller for otherwise hands-free image manipulation or temporary reversion to telephone use.
Watch this space!
Dr. Alan Johnston is a former Reader and Associate Professor in the Department of Optometry at the University of Melbourne. He was one of the first sessional optometrists at the Kooyong Low Vision Clinic of the Association for the Blind, and an organiser of the 1980 and 1990 Low Vision Ahead Conferences, events that established the world’s premier triennial low vision conference. Dr. Johnston became a Fellow of the American Academy of Optometry in 1968 and a Diplomate of the Low Vision Section of that Academy in 1985. He is one of only three clinical Diplomates of that section from outside North America. Dr. Johnston established Alan Johnston Vision Consulting in 2002 to provide advice on magnification and visual ergonomics to industry and vision service organisations. He develops custom vision devices for magnification in commercial applications and offers advice on vision use and efficiency in industry. Dr. Johnston is a regular academic visitor to the Wenzhou Medical University and the Tianjin Eye Hospital in China.
Reference
1. http://www.thelancet.com/journals/lancet/article/PIIS0140-6736(15)61340-X/abstract